Dr. Miguel Ángel Rodriguez
Endoscopy of the spinal column
Minimally invasive technique in just 60 minutes
Dr. Miguel Ángel Rodriguez
Specialist in Endoscopic Spine Techniques
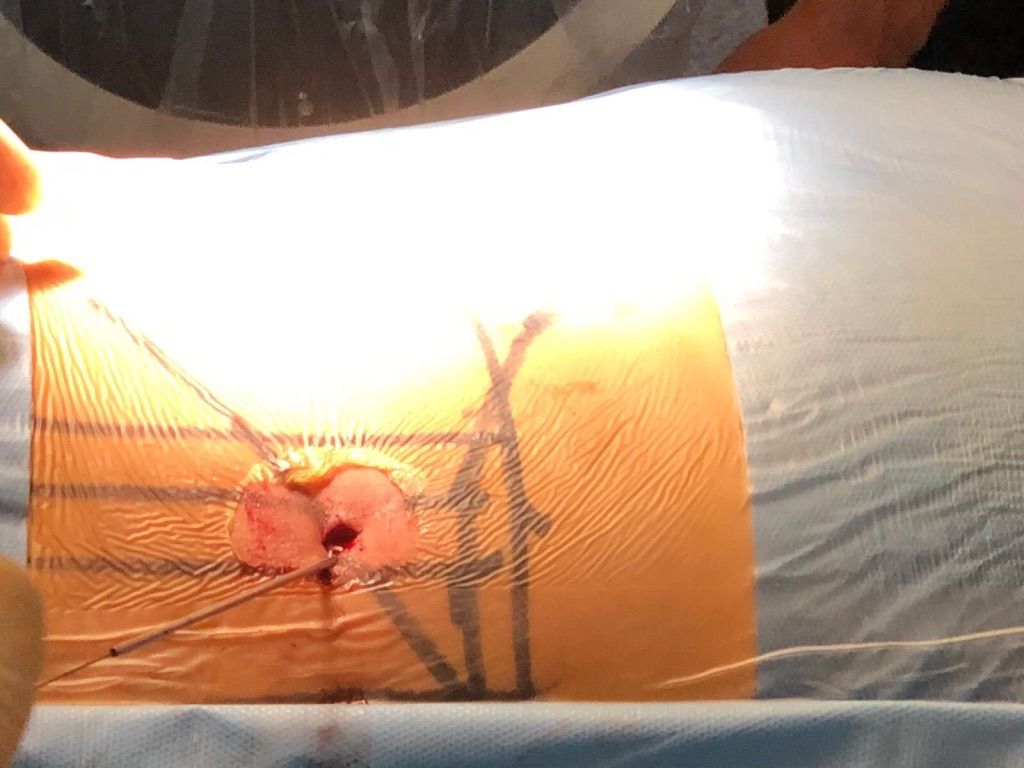
Spinal endoscopy is a minimally invasive technique at the forefront of spinal surgery. With a 0.8 mm surgical approach and a high-definition endoscopy system, we perform surgical treatment of the most prevalent pathologies in our environment, such as disc herniation, foraminal stenosis, canal stenosis, facet hypertrophy, etc.
Case 1
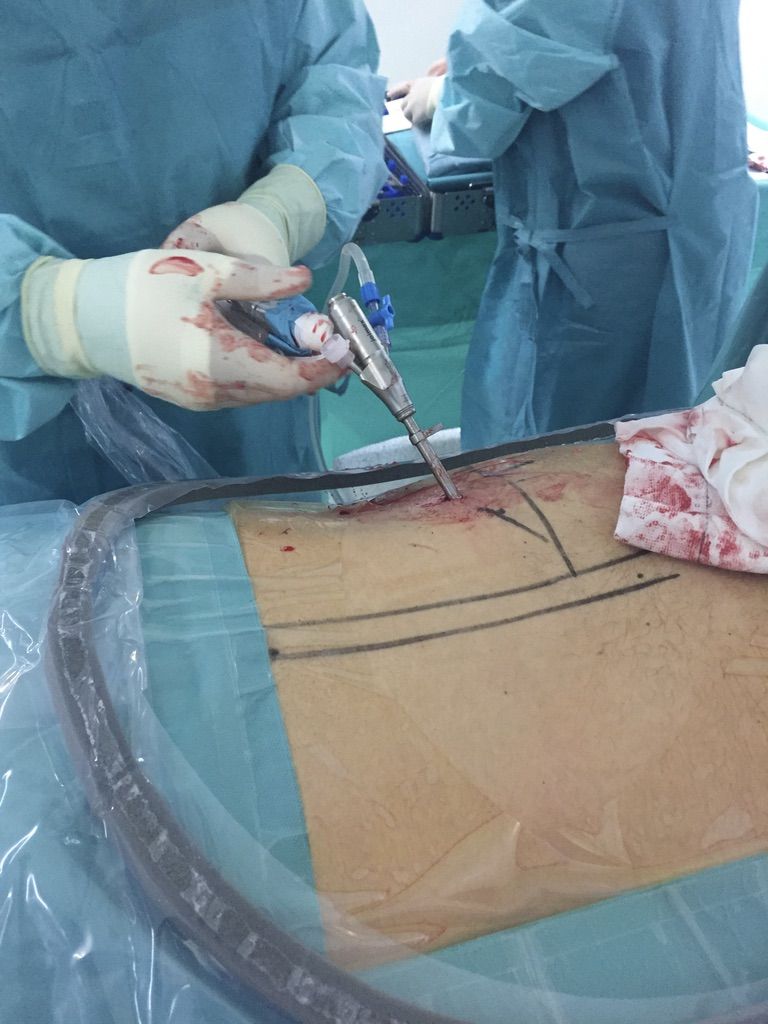
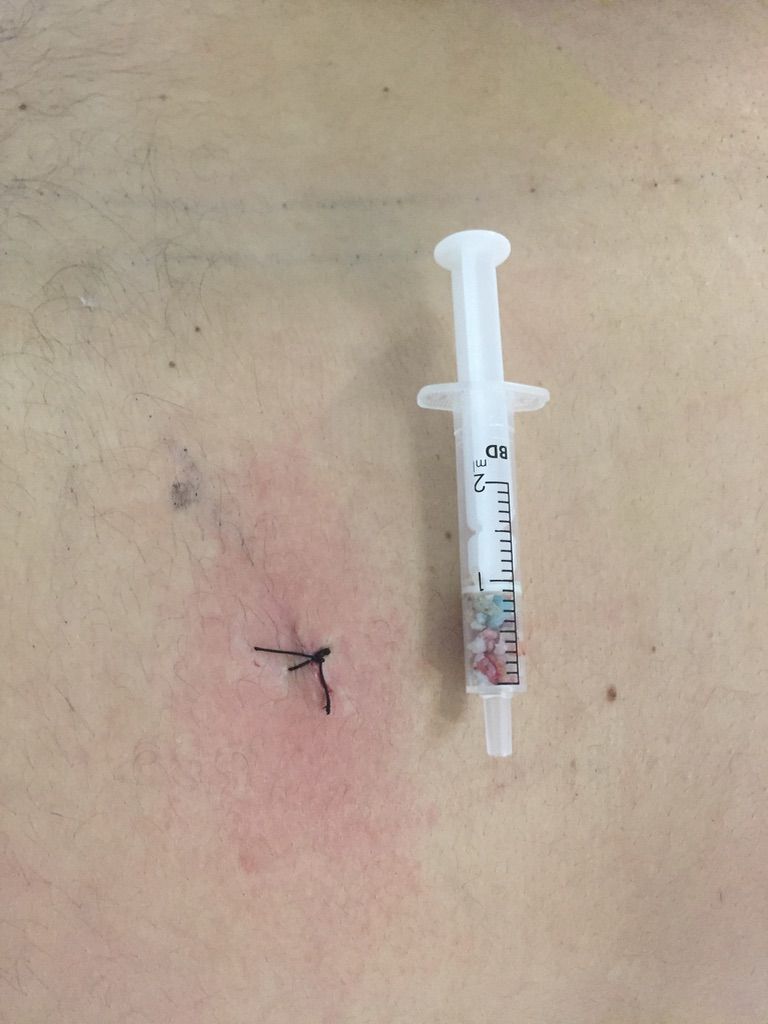
How is the Technique Performed?
Patient anaesthesia, always at the anaesthesiologist’s discretion, depending on the anaesthetic risk ASA in most cases is general anaesthesia, although in certain cases it can be performed with spinal anaesthesia or local anaesthesia with sedation.
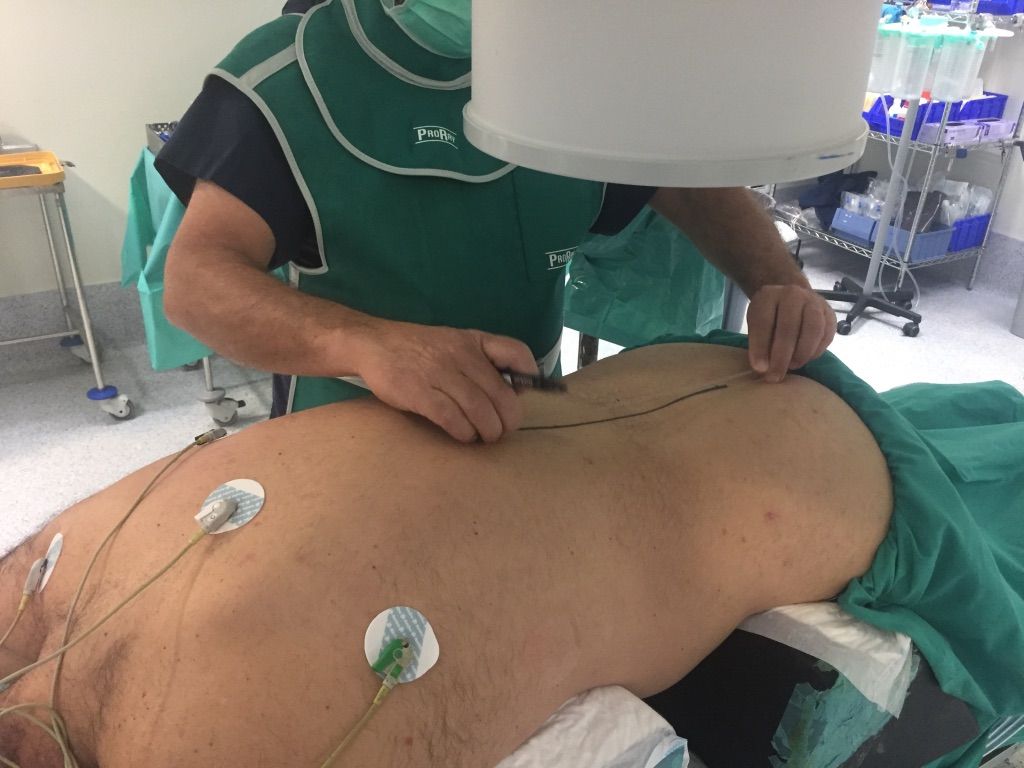
Patient positioning for this technique is performed in prone or lateral decubitus.
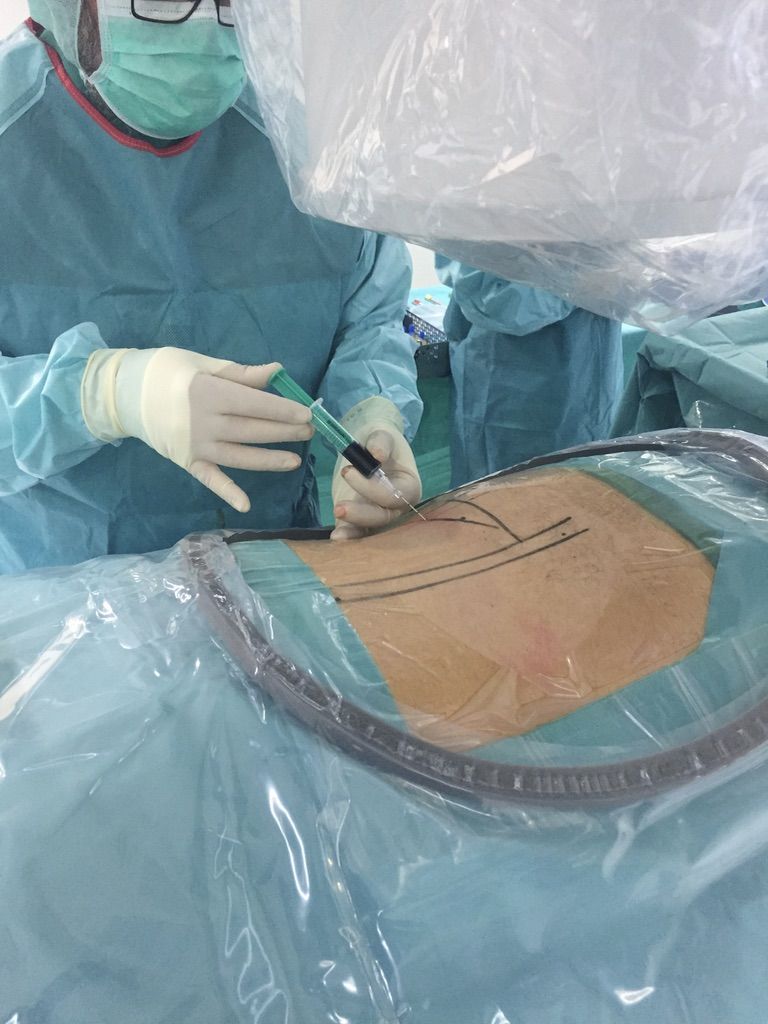
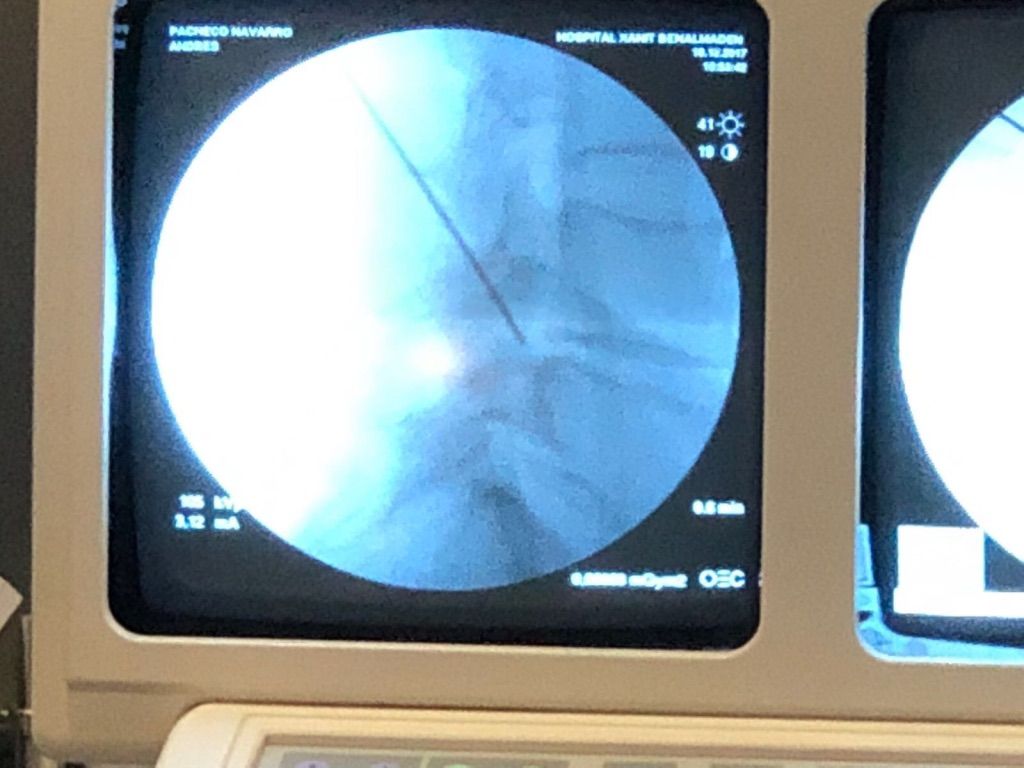
Surgical access by image intensifier (X-ray) control.
The surgical time for the endoscopic technique is around 60 minutes.
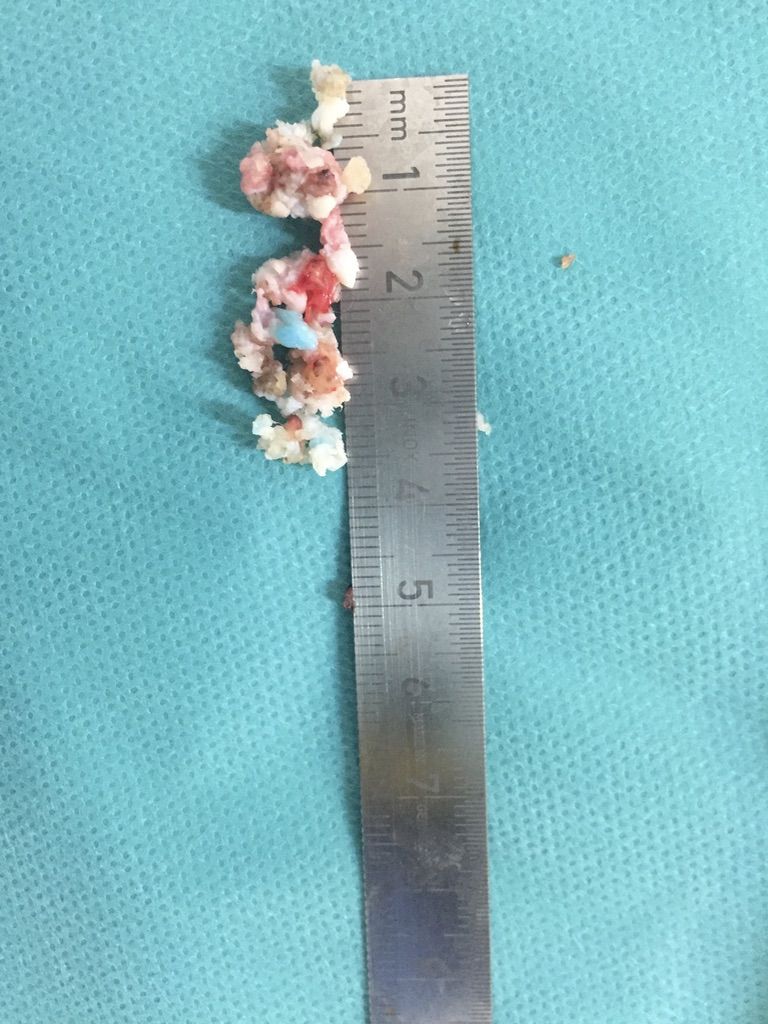
Video of foraminal stenosis and removal of disc material, foraminal braking and descending root release.
Clinical Cases
Spine Endoscopy

Case 1
Male, 57 years old
6 weeks with right L5-S1 radiculopathy, no improvement with analgesic treatment (NSAIDs, neurolytics, etc.).
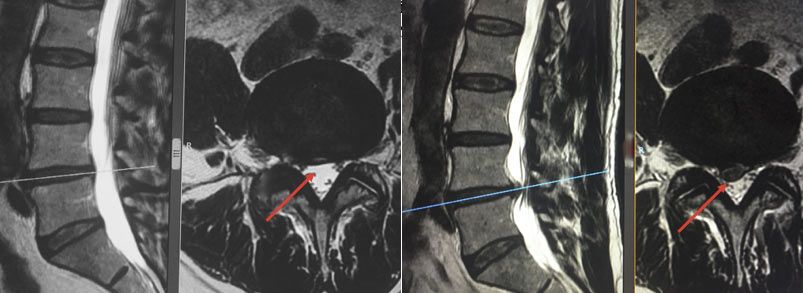
MRI large right L5-S1 disc herniation with acute and severe S1 radicular involvement.
Oswestry 58 VAS 9 in right lower limb.
Image: 6 weeks after surgical intervention Oswewtry 20. VAS 2
Case 2
Male, 41 years old
3 months with right L4-L5 radiculopathy, without improvement with analgesic treatment (NSAIDs, neuroleptics, etc.).
MRI scan of right paracentral disc herniation L4-L5 right with chronic and severe radicular involvement.
Oswestry 76 VAS 8 in right lower limb.
Sporting activities 3 months, return to work 4 weeks.
Image: 3 months after surgery. Oswewtry 18. VAS 2

Case 3
Male, 57 years old
- Lumbar arthrodesis L5-S1 10 years ago
- 3 years with right L4-L5 radiculopathy, no improvement with analgesic treatment (NSAIDs, morphic patches, neurolytics, peridurable infiltrations by pain unit…)
- Development of adjacent syndrome after arthrodesis 10 years ago.
Image: Oswestry 68 VAS 8 in right lower limb.
Endoscopic Spine Surgery
What does Spine Endoscopy consist of?
Spinal endoscopy is a minimally invasive technique at the forefront of spine surgery. With a surgical approach of 0.8 mm and a high-definition endoscopy system, we perform surgical treatment for prevalent conditions in our field, such as disc herniation, foraminal stenosis, hypertrophic facet joint stenosis, and more.
The technological advancements in endoscopy systems over the last 30 years have allowed for the evolution of surgical techniques with multiple possibilities for accessing lumbar and cervical pathologies.
The constant innovation of Joimax endoscopes enables access to high-resolution images of the spinal canal area and manipulation of the intervertebral disc, dural sac, and nerve roots through its monotube system.
The use of TESSYS and ILESSYS systems allows for transforaminal and interlaminar access, respectively, to distinct levels and lumbar and cervical pathologies.
What type of patients are candidates for Spine Endoscopy?
The age range of candidates for this technique is extended compared to traditional open surgery, thanks to reduced surgical time and less anatomical trauma. This means that elderly patients with underlying conditions who would not be candidates for conventional surgery can now be considered.
A thorough preoperative evaluation is essential and should include not only the patient’s symptoms, which are mandatory, but also the following complementary tests: lateral and anteroposterior X-rays, magnetic resonance imaging (MRI), and a neurophysiological study with electromyoneurography.
Before deciding to perform surgery, the patient should have experienced symptoms related to lumbar disc herniation or foraminal stenosis for approximately 6 weeks without evident clinical improvement, based on Oswestry tests. However, each case is individually evaluated.
How is the technique performed?
Anesthesia for the patient is always determined by the anesthesiologist, considering the ASA (American Society of Anesthesiologists) anesthesia risk classification. In most cases, general anesthesia is used, although in specific situations, spinal anesthesia or local anesthesia with sedation may be considered.
The patient’s positioning for this technique is typically done in a prone (lying face down) or lateral (lying on the side) position.
Surgical access is achieved under fluoroscopy or X-ray guidance to ensure precision.
The surgical duration for the endoscopic technique typically lasts around 60 minutes.
Postoperative and return to daily activity
The postoperative period typically lasts for 24 hours, although patient mobilization and walking usually begin within 6-8 hours.
Pain tends to disappear immediately after surgery.
It is not uncommon for patients to experience paresthesias (tingling sensations) after surgery, which gradually subside over a few weeks.
Patients are discharged from the hospital on the same day as the operation or the following day, once they have recovered from anesthesia.
It is advisable to wear a lumbar support belt for the first two weeks and avoid physical exertion for about a month after surgery.
The surgical incision does not require specific care. It should be kept clean and dry, and sutures are typically removed after one week.
In which pathologies is Spinal Endoscopy the Gold Standard?
The technological advancements in current endoscopy systems and the extensive learning curve in the management of arthroscopic systems and minimally invasive spinal surgery make it possible to treat conditions such as:
– Disc herniation, intracanal, intraforaminal, and extraforaminal
– Canal stenosis and foraminal stenosis
– Adjacent segment syndrome
– Juxtafacet cysts
– Discitis
How does Endoscopic Spine surgery improve over open surgery?
Due to the minimal tissue damage and preservation of anatomical structures, recovery after surgery is quicker with minimally invasive spinal endoscopy. Patients can return to their daily, work, and sports activities more rapidly.
The risk of infection is reduced compared to microsurgery due to the small incision used in advanced spinal endoscopy.
These procedures often qualify as day surgery, with a hospital stay of less than 24 hours.
There is a lower risk of degenerative complications since the goal is to restore the original anatomy without the use of instrumentation like screws, plates, or rods.
The procedure results in minimal bleeding compared to open surgery, allowing for treatment in elderly patients and those with overall health instability.
Clinic
Medical Centre
MedHelp Marbella
medhelpmarbella@gmail.com
Appointment Times
Mon-Fri: 9:30-3:00pm
Mon & Thur: 4:00-8:00pm