Dr. Miguel Ángel Rodriguez
Sports Traumatology
Specialist in Injuries and Innovative Treatments
Dr. Miguel Ángel Rodriguez
Specialist in Sports Traumatology
Sports injuries have increased in recent years due to the demands placed on the body and the increasing age of sportsmen and women. Some injuries are caused by trauma or accidents. However, most injuries involve constant overexertion of the locomotor system.
The traditional attitude of Traumatology and Orthopaedic Surgery has been to consider amateur sports practice as something dispensable. Often the first recommendation received by patients was to give up their favourite sport. Regular exercise is now considered advisable for the physical and emotional health of any person, so the functional recovery of the patient deserves the same care as the most professional sportsperson. Sports traumatology has come a long way in recent years, with earlier diagnoses, more precise recommendations, and sometimes surgical interventions that allow sufferers to continue practising sport.
Treatments
Treatment in Young Athletes
Musculoskeletal injuries produced during sports practice in this age group have different connotations with respect to adults. On the one hand, they are based on immature systems, more sensitive to impacts and overload injuries. On the other hand, the biological potential for tissue regeneration is greater and faster than in adults, so healing is usually faster and more complete.
A characteristic injury of the infantile and juvenile skeleton is the injury of the growth plate, medically referred to as epiphysiolysis. Growth plates are unossified points of bone, so infant fractures often occur at these weak points. Injuries to the growth plate require specific and careful treatment, because they can alter the further development of the affected bone.
At the amateur level, it is often necessary to modify or redirect sports practice, because some patients have a greater predisposition to suffer certain injuries, which can greatly reduce the athlete’s performance and future expectations, leading to an early withdrawal from a promising career. It is increasingly common to see cases of children and adolescents with significant family pressure, or pressure from their close environment, to increase their sporting performance as a way of saving the family’s economic or social situation. These sportsmen and sportswomen should be specially counselled in planning their sporting future. Fighting against nature sometimes only leads to frustration, and at a young age, new sporting routines adapted to the patient’s physique can be established with a high chance of success.
Treatment in Adult Athletes
The most common sports injuries in adults affect muscles, tendons, ligaments and bones.
The stages in the evolution of any injury (wound, fracture, sprain,…) are as follows:
Immediately after trauma, there is a rupture of structures, including blood vessels, with bleeding, haematoma and inflammation. The temporal duration of this phase varies depending on the tissues involved, type and severity of the injury.
Almost at the same time and overlapping the initial phase, the inflammatory reaction initiates the phase of cell stimulation, stem cells, fibroblasts, etc., which are the “workers” that will provide new materials (extracellular matrix, collagen fibres, bone tissue, etc.), necessary for repair.
The accumulation of cells and tissue is what forms the “scar” (or bone callus in fractures). The final phase is the remodelling and maturation of the scar tissue. Here, tissue adaptation to biomechanical requirements takes place, eliminating excess tissue production and aligning fibres and tissue resistance to the lines of forces to which it is subjected.
These general phases, which occur to a greater or lesser degree during the healing of any damaged tissue, have differentiating characteristics depending on the age of the athletes, whether the trauma is high or low energy, whether it involves tendon, muscle or bone.
The predominance or absence of any of these processes during healing will depend on the treatment applied from the onset of inflammation, from which it follows that we should not try to block inflammation but to channel it (current concept of bioregulation of inflammation).
The application of local cold has an analgesic effect and reduces inflammation. From this point on, the application of local heat increases the healing capacity by increasing vascularisation in the focus of the injured tissue.
Medicinal measures, physiotherapy, are carried out during the healing phases after the healing process has been completed. Sports rehabilitation is necessary for the return to sport after complete recovery of joint mobility and muscle power.
Innovative Treatments
Hyaluronic acid
Hyaluronic acid (HA) is part of the connective tissue (it is a fundamental component of the extracellular matrix) and of the synovial fluid (increasing its viscosity). Skin and cartilage are two tissues rich in hyaluronic acid and it plays an important role in them. HA plays an important role in the repair processes of wounds and skin damage.
The use of HA in the form of intra-articular injections in patients with osteoarthritis of the knee (gonarthrosis) was called viscosupplementation and was the first indication in traumatology. The purpose of this treatment is to achieve a lubricating, mechanical and biochemical effect on the joint affected by osteoarthritis, resulting in at least partial relief of painful symptoms and improved function. The effect is usually not immediate but long-term. Studies have demonstrated its efficacy and safety, improving pain and function and delaying the implantation of a prosthesis in patients with severe osteoarthritis of the knee.
In recent years, HA injections have been extended to other joints, such as the ankle, hip, shoulder and even small joints of the hand or temporomandibular joint.
Oral HA preparations are now also available for the treatment of patients with osteoarthritis and articular cartilage diseases. The efficacy is not completely proven, side effects are not relevant.
Intra-articular injections of hyaluronic acid are a common treatment in our daily clinical practice. We use viscosupplementation in joints affected by degenerative changes, osteoarthritis or chondropathy. The knee is the joint that most frequently receives this treatment, but we also use it in ankle, hip, shoulder, elbow, wrist, and even in joints of the hand or foot. We also use HA in infiltrations together with corticoids in patients with joint pain without significant anatomical lesions or in whom conservative treatment is not useful.
Finally, in many arthroscopic operations, hyaluronic acid infiltration is being tested at the end of surgery to accelerate the recovery of joint fluid characteristics.
Oral supplements of hyaluronic acid and chondroprotectors such as chondroitin and glucosamine may be recommended in patients with mild symptoms and in all those operated on with cartilage pathology. While these appear to be effective in reducing inflammatory and painful symptoms, it is unclear whether they will reduce the progression of degenerative pathology.
In patients with patellar chondropathy it is more common to do several infiltrations, every week or every two weeks to see the evolution and progressive improvement.
No major adverse reactions are usually found after HA injections, although in some cases the patient has pain a few hours or days after the intra-articular injection.
Frequent Injuries:
Muscle Injuries
Fibrillary Rupture
Muscle develops in response to training and atrophies when there is excessive rest or it is immobilised.
Muscle injuries are very common in sport and although they are not usually serious, they must be studied and treated seriously, as the most frequent complication is relapse, often due to the athlete’s own impatience. They can compromise recovery times, planned competitions and make the patient who suffers from them despair.
A history of sudden pain (pulling) and inability to continue with exercise is diagnostic of muscle rupture. There is not always obvious bruising of the skin, and if it appears it is usually after several hours or a few days.
Muscle rupture is common in explosive movements, speed and changes of rhythm. They are more frequent in older athletes, and in those who have less sporting practice or make mistakes in the preparation of the exercise. The most frequently injured muscles are the calf and soleus, the hamstrings, the anterior rectus quadriceps and the adductor magnus. But muscle tears can be seen in any muscle of the lower limb, in the abdominals or in the arm musculature.
The calf muscle rupture is so common in racket sports that it is referred to in English literature as a “tennis leg”. The soleus suffers in middle-distance and long-distance runners, and the hamstrings are more commonly damaged in sprinting and hurdling. The rectus anterior quadriceps is most commonly injured in football players.
There are three grades from minor (grade I) to major (grade III). Imaging tests allow the prognosis and treatment plan to be established. Ultrasound is cheaper and more dynamic, but its assessment is more dependent on the experience of the person performing it. Magnetic resonance imaging allows for better anatomical detail and to see the muscle oedema produced by the injury.
In mild to moderate injuries (most), rest is only necessary for the first 48-72 hours. During this period, cold is applied and, if necessary, the area is immobilised.
Subsequently, controlled, non-painful movement is best. Non-load-bearing exercises such as swimming or cycling should be started as soon as possible.
Physiotherapy is very important to speed up recovery. Drainage techniques are used, techniques that facilitate healing are applied, and then the area is relaxed and a return to normality is encouraged.
All of the above is incomplete if there is no subsequent progressive strengthening and re-education of activity prior to the return to normal sporting activity. This aspect is often forgotten and is a frequent cause of relapses.
Among the complications of muscle ruptures, in addition to ruptures, we can mention the formation of a painful scar, the encapsulation of a haematoma or its calcification.
We must stress the importance of prevention, which basically consists of muscle strengthening work, stretching after exercise, rest, massage, correct hydration and nutrition, in short, everything that has come to be known as “invisible training”.
Chronic Compartment Syndrome
The muscles of the body are grouped into compartments that are wrapped in a connective tissue that acts as a sheath for them and is called fascia. When we exercise, the muscles work and receive more blood flow, increasing their volume. The capacity for distension of the fascia that surrounds the muscle is limited, and in some cases pain may appear in relation to exercise, due to a process in which the pressure inside the compartment is higher than normal, preventing normal blood flow to the muscle. With rest, the pressure normalises and the pain disappears.
This phenomenon is more common than it might seem. The most common compartments that are the seat of this syndrome are those of the leg and forearm. Chronic posterior compartment syndrome of the lower leg occurs mainly in runners. The pain in the calf makes it impossible to continue running. The pain comes on with exercise, gets worse if the pace is maintained, and only gets better when stopping. It can be superficial when it affects the compartment that houses the calf muscles, or deep, if it affects the tibialis posterior and the flexors of the toes.
The most common one seen in long-distance runners and walkers is anterior compartment syndrome of the leg, which affects the tibialis anterior muscle that extends the ankle with each step when walking. The symptoms are sometimes confused with those of “periostitis”.
Chronic compartment syndrome of the forearm is suffered by athletes such as motorcyclists or climbers who make continuous efforts with this musculature.
Conservative treatment can be helpful in the early stages, before it becomes a chronic problem. Massage and stretching, relative rest of the muscle group, cold, and other physiotherapy techniques may help. If the patient does not improve, chronic compartment syndromes require surgical treatment consisting of a fasciotomy. In this procedure, the fascia is opened so that it no longer compresses the affected muscle. Through small incisions the fascia is opened and the recovery process is relatively quick, once the stitches are removed, exercise can be resumed progressively. The results are good and only in some cases relapses occur.
Tendon Injuries
Achilles tendon
The Achilles tendon or calcaneal tendon is the most powerful tendon in the human body. It is the tendon of the triceps suralis muscle of the leg, made up of the calf and soleus muscles. It inserts at the back of the calcaneal bone, at the level of the heel. The main function of this tendon is plantar flexion of the ankle, propelling us in walking, running and jumping. It supports forces of up to 10 times body weight in these activities.
The Achilles tendon is about ten centimetres long and approximately one centimetre wide in its central third, where its section is more circular.
We could classify Achilles tendon injuries into two groups:
Tendon ruptures, they are usually acute, very disabling, and in many cases are treated surgically.
Tendinopathies. We have abandoned the term tendinitis because there is almost never very evident inflammation, except at certain times. They are more related to overuse, almost always in sports in which running and jumping predominate. They are also seen in sedentary middle-aged people. Conservative treatment resolves most cases.
When the Achilles tendon ruptures, it often ruptures completely and abruptly. Most often, the patient feels a sharp, sharp pain, with the sensation of being kicked from behind. From that moment on, they can no longer continue with their activity, and can hardly walk.
Many of the athletes who suffer this injury had no previous discomfort in the tendon. Others played sport sporadically, but did not carry out a strengthening and stretching programme, which to a certain extent prevents this pathology. It is common in football, basketball, squash, tennis, sprinting and jumping.
Degeneration of the tendon tissue has been shown to be a major factor favouring the injury. The term for this degeneration is “tendinosis”.
An experienced orthopaedic surgeon can diagnose the rupture simply on the basis of the patient’s history and physical examination. However, ultrasound or MRI scans are often performed to determine the exact type and location of the injury and to plan the most appropriate treatment.
Surgical treatment allows for a somewhat faster recovery and fewer relapses. In cases of patients with a high surgical risk that contraindicate the patient undergoing surgery, treatment consists of immobilisation (about 6 weeks) and subsequent rehabilitation.
The vast majority of patients undergo surgery. Open repair is the most commonly performed technique. Termino-terminal repair of the tendon is almost always possible, with adequate suturing of both tendon ends. In some patients with extensive degeneration or destructuring, it may be necessary to use donor grafts, or plasties from the patient’s own triceps fascia or the tendon of the plantar thin muscle.
In about 3-4 months the patient recovers normal physical activity, although full recovery may take up to a year, although this is achieved in a large percentage of cases. Rehabilitation is essential to achieve a good result.
There are early postoperative complications (infection, thrombosis, wound dehiscence) and late complications (rerupture, loss of strength or limited mobility of the ankle).
There are some cases in which the rupture was not detected or was treated conservatively, with poor evolution. These are called chronic ruptures, and the surgical technique is similar, with the use of grafts or plasty with adjacent tendons being more often necessary in this case.
Noninsertional Achilles Tendinopathy
This is the name given to chronic pain in the middle third of the tendon. It is common in runners, due to overload, but it is also seen in sedentary people, with some favourable factors such as overweight and diabetes.
Supplementation with some nutrients such as hyaluronic acid, collagen, antioxidants and essential fatty acids seem to improve symptoms, although there is no clear evidence of their benefits.
The pathological process is usually always associated with chronic inflammation and thickening of the tendon sheath or peritendon (chronic peritendinitis), and degeneration of the connective tissue in the body of the tendon (tendinosis).
Diagnosis is easy with pain on palpation, fusiform thickening of the tendon, or presence of nodules. Ultrasound or magnetic resonance imaging helps to define the state of the tendon, and to assess whether there is a rupture or intratendinous cyst.
In acute phases, treatment should be based on conservative measures: cold, elevation, compression and short periods of rest. In amateur athletes, it is often necessary to temporarily modify sporting activity until the symptoms disappear completely. In runners, symptoms are reduced or disappear when cycling, swimming or cycling on the elliptical trainer.
The basic treatment is physiotherapy and sports re-education. Exercises with progressive loading and stretching are the basis. Therapies such as extracorporeal shock waves or EPI can be tried. Effectiveness varies greatly from patient to patient. Platelet growth factor or platelet-rich plasma (PRP) infiltrations are being used, with promising results, although more experience is needed for widespread recommendation.
Surgery is indicated after 6 months of well-conducted conservative treatment without satisfactory results. The techniques consist of freeing the tendon from the adhesions that cover it, opening the fascia and peritendon, and in cases of tendinosis, resecting the pathological areas and performing longitudinal tenotomies to stimulate the self-repair process. Surgery is rarely necessary in amateur athletes, and requires long convalescence in professional athletes.
Return to normal life takes around 4-6 weeks, but normal physical activity should be resumed very slowly, with special emphasis on strengthening and maturation of the operated tendon tissue. The previous level may take about a year to reach. The tendon is thickened after the operation but is no longer painful.
Chronic Insertional Tendinopathy
On other occasions, the origin of Achilles tendon pain is in its most distal part, where it inserts into the calcaneus. In this area, there may be tendon degeneration (tendinosis, sometimes with partial tendon tears), or sometimes inflammation of the retrocalcaneal bursa (Achilles bursitis). Intratendinous calcifications are common, resembling a spur at the insertion site. The upper edge of the calcaneus can become very prominent and leave an imprint on the tendon, especially during ankle dorsiflexion.
As in non-insertional tendinopathy, cases can occur in athletes due to overuse or in sedentary middle-aged patients with overweight. In the initial episodes of pain, rest, local cold application, and anti-inflammatories often provide significant relief of symptoms. If the process becomes chronic, the chances of rapid improvement with conservative treatment decrease.
Options for walking and running without pain decrease, and the activity must be modified, with swimming and generally cycling being well-tolerated. Conventional physiotherapy can help control pain.
The heel should always be examined carefully, distinguishing all the areas that can be a source of pain. Regarding complementary examinations, a lateral X-ray of the calcaneus shows the shape of the calcaneus and the presence or absence of calcification. To assess the bursa and the tendon, an ultrasound or magnetic resonance imaging (MRI) is also necessary.
In cases of bursitis, corticosteroid injection is very useful. The Achilles tendon itself should not be injected with corticosteroids, as it can weaken its strength and promote tendon tears. For partial tears or tendinosis, injection with Platelet-Rich Plasma (PRP) reduces symptoms and seems to aid in faster regeneration.
In cases of significant tendon calcification or Haglund’s disease (calcaneal exostosis), surgical intervention may be an option to alleviate symptoms. The operation involves resecting the prominence of the calcaneus and any existing calcification. Percutaneous treatment (minimally invasive surgery) is feasible for removing Haglund and the bursa but not for extracting intratendinous calcification or treating tendinosis and insertional tendonitis. In these cases, the tendon is approached longitudinally, and if there is significant degeneration and weakening of the insertion, it is reattached with suture anchors.
Load-bearing should be progressive, but sometimes it is delayed for a few weeks if the tendon was severely damaged and needed reattachment. Walkers or walking boots are used during the transition from unloading to resuming normal life, with the advantage of being removable for sleeping and hygiene. The return to sports is gradual, starting with cycling and swimming, followed by strength training in the gym, and finally by progressive running. Depending on the type of surgery, recovery to the previous level can be achieved between 6 months and a year.
Peroneal tendons
The tendons of the peroneal muscles are located on the lateral and distal side of the leg, running behind the outer ankle malleolus towards their insertions in the foot.
The long peroneal tendon runs towards the sole of the foot and crosses it, inserting into the plantar region of the base of the first metatarsal and the first wedge.
The short peroneal tendon inserts into the base of the fifth metatarsal of the foot.
The main function of these muscles and tendons is the eversion movement of the foot, which combines abduction and external rotation of the foot. They are essential for the dynamic stabilization of the ankle.
Injuries to these tendons can be summarized as follows:
Overuse injuries: tendinopathy and tenosynovitis. Traumatic injuries: dislocation of the peroneal tendons and their rupture.
OVERUSE INJURIES
The peroneal tendons can frequently develop inflammation of their synovial sheath, referred to as peroneal tenosynovitis. It usually occurs after an overload or effort that triggers inflammation. This process can also be seen in patients with rheumatic and systemic inflammatory diseases.
Clinical diagnosis can be made based on pain and swelling along the peroneal tendons. Diagnosis can be complemented with ultrasound or magnetic resonance imaging (MRI).
Initial treatment consists of rest, elevation, and local cold application. Subsequently, anti-inflammatory physical therapy may be useful, which can be combined with oral medication for that purpose.
If there is severe or treatment-resistant pain, local injection with corticosteroids into the sheath can quickly resolve the condition.
In some cases, pain is not accompanied by obvious inflammation, and this is referred to as peroneal tendinopathy. Peroneal tendons can undergo a degenerative process called tendinosis, which involves alterations in the structure and architecture of collagen fibers in the tendons. The cause of this condition may be related to biomechanical abnormalities in gait combined with high exercise loads.
Physical therapy plays a fundamental role in the recovery from these injuries. Once pain is under control, it is essential to perform appropriate strengthening and proprioception work. Identifying and correcting factors that may have triggered the condition is crucial. Evaluating the correction of gait with orthotics is common in these patients.
If the condition does not improve after several months of treatment, surgical intervention may be necessary, either endoscopic (arthroscopy or tenoscopy) or open surgery, to perform synovectomy, clean, and review the peroneal tendons. It is a simple procedure with rapid recovery.
DISLOCATION AND RUPTURE OF THE PERONEAL TENDONS
The most characteristic traumatic injury to the peroneal tendons is their dislocation, where they come out of the osteofibrous tunnel that surrounds them following indirect trauma, with a sudden twist of the foot that breaks or tears the retinaculum that encloses the tendons, causing them to dislocate anteriorly over the crest of the fibula.
This initial episode is often initially confused with an ankle sprain, and if the extent of the injury is not identified in the emergency room, the possibility of recurrent dislocations is high.
The treatment of choice is surgical, involving the repair of the retinaculum that must be reattached to the fibula, repositioning the tendons in their retromalleolar location, and repairing any tendon injuries if present. The use of crutches and immobilization for 2-3 weeks is necessary. Walkers or walking boots are used during the transition from unloading to normal life, with the advantage of being able to remove them for sleeping and hygiene. The return to sports is gradual, starting with cycling and swimming, followed by gym strengthening, progressive running, and then contact sports.
Please note that this translation is for informational purposes and should not replace professional medical advice.
Patellar Tendon
Patellar Tendon: Structure and Function
The patellar tendon, also known as the patellar or kneecap tendon, is one of the most powerful tendons in the human body. It measures approximately 4 to 5 centimeters in length, about 3 centimeters in width, and roughly 1 centimeter in thickness. It’s considered part of the knee extensor apparatus, consisting of the quadriceps muscle, its quadriceps tendon, the patella (kneecap), and the patellar tendon, which inserts into the tibia.
This tendon plays a crucial role in maintaining an upright posture against gravity, which is essential for activities like walking, running, and jumping.
Types of Patellar Tendon Injuries
Patellar tendon injuries can be classified into the following groups:
Tendon Ruptures: These are usually acute, highly disabling injuries that almost always require surgical intervention.
Tendinopathies: These are typically chronic conditions. The term “tendonitis” is no longer used because inflammation is rarely the main issue, except in some cases. These injuries are often related to overuse, particularly in sports that involve running and jumping. Conservative treatment is effective in most cases.
Patellar Tendon Ruptures
When the patellar tendon ruptures, it usually happens suddenly and completely. The most common symptom is intense, sharp pain, often accompanied by the sensation of the tendon tearing. Following the injury, walking becomes impossible. In older athletes, a rupture of the quadriceps tendon above the patella is more common.
Many athletes who suffer this severe injury had no prior symptoms in the tendon. Most of them engage in sports on weekends or sporadically without following a strengthening and stretching program, which can prevent such injuries. While patellar tendon rupture is rare, it can occur in sports like football, basketball, handball, squash, or during high-impact activities.
Tendon degeneration has been identified as a key factor that increases the risk of this injury. The term used to describe this degeneration is “tendinosis.”
Experienced orthopedic surgeons can diagnose patellar tendon rupture based on the patient’s history and physical examination, which may reveal patellar elevation. However, ultrasound or magnetic resonance imaging (MRI) is routinely performed to assess the extent of the tendon injury.
Surgical treatment is the most effective approach. In cases where surgery poses significant risks, immobilization (approximately 6 weeks) followed by knee rehabilitation is considered. The majority of patients undergo surgery, with open repair being the technique that yields the best results in terms of returning to their previous level of physical activity. Ruptures usually occur near the bone, so the repair involves reattaching the tendon to the lower pole of the patella and reinforcing that area. In some cases with extensive degeneration, grafts or grafting from adjacent tendons like the semitendinosus may be necessary.
The knee is immobilized for several weeks, and subsequent rehabilitation is essential for a successful outcome.
Postoperative complications can be either early (infection, thrombosis, wound dehiscence) or late (re-rupture, loss of strength, or limitations in knee flexion and extension).
In cases where the rupture is not detected or appropriately treated initially, the surgical technique is similar, but grafts or grafting from adjacent tendons are more frequently required.
Patellar Tendinopathy
Chronic pain in the patellar tendon is referred to as patellar tendinopathy. It is common in sports that involve running and jumping and is considered an overuse injury. The most typical location of pain is the proximal (near the top) part of the tendon where it attaches to the patella. This condition is often called “jumper’s knee” and is prevalent among volleyball players, basketball players, tennis players, and runners.
Symptoms improve with periods of rest but return or worsen when the individual resumes normal activities.
The underlying pathological process involves degeneration of the connective tissue within the tendon (tendinosis), typically in the deeper and upper part of the tendon.
Diagnosis is straightforward and involves pain upon palpation, fusiform thickening of the tendon, or the presence of nodules. In cases of acute peritendinitis, there may be crepitus with movement. X-rays of the knee are always taken to assess patellar morphology and position. Ultrasound or magnetic resonance imaging helps define the tendon’s condition, determine if there is a rupture or intratendinous cyst, evaluate peritendon thickening, and check for the presence of fluid between the peritendon and tendon. MRI can also reveal associated intra-articular injuries.
In the acute phase, treatment is based on conservative measures like ice, elevation, compression, rest, or activity modification. Jumping motions should be avoided while symptoms persist.
In cases of severe pain and the need to participate in competitions, corticosteroid injections may be used exceptionally, although they may weaken the tendon and increase the risk of rupture.
Physical therapy that has proven effective in treating this condition involves daily eccentric exercises lasting 6 to 12 weeks, progressively increasing the load. This regimen includes slow descents using only one leg (eccentric work).
Additional physical therapy techniques, such as extracorporeal shockwave therapy or EPI (percutaneous electrolysis), may be combined.
Injections with platelet-rich plasma (PRP) are theoretically useful for accelerating the regeneration of tendinosis areas or healing ruptures. However, there is still not enough experience to make widespread recommendations.
Surgery may be considered after 6 months of successful conservative treatment in patients who do not want to modify their sports activities. Surgical techniques involve freeing the tendon from any adhesions, excising pathological areas in cases of tendinosis, and performing longitudinal tenotomies. In cases of calcifications or exostoses, these can be removed to prevent irritation. Knee arthroscopy is recommended to rule out other causes of anterior knee pain, often associated with patellar cartilage damage.
Returning to a normal life takes approximately 6 weeks, but physical activity should be gradually reintroduced, with a focus on strengthening and maturing the operated tendon tissue. It may take up to a year to return to the previous activity level, although running can begin earlier. The tendon becomes thicker after surgery but is no longer painful. The rehabilitation period for high-level athletes can be quite long.
Ligament Injuries
Rupture of the Anterior Cruciate Ligament of the Knee
Knee Crossed Ligaments: Anatomy and Injuries
The crossed ligaments of the knee are two ligamentous structures located within the joint, connecting the femur and tibia to provide stability in the anteroposterior direction of one bone over the other. The anterior cruciate ligament (ACL) runs from the posterior and outer part of the intercondylar notch of the femur to its anteromedial insertion on the tibia. It crosses in front of the posterior cruciate ligament (PCL), which runs in the opposite direction, from the anterior and medial part of the femoral notch to the posterior region of the tibia.
The cruciate ligaments are essential for the proper kinematics of the knee. The ACL is frequently injured due to knee twists, especially in sports involving pivoting with the foot planted, such as soccer, basketball, handball, skiing, and more. It is also commonly injured in combat sports like judo and in motocross or trials when there is sudden foot impact on the ground.
Most of the time, a complete tear of the ligament occurs, which detaches or ruptures at its femoral or proximal insertion. In many cases, ACL injury is accompanied by injuries to the medial collateral ligament, meniscal injuries, and bone contusions on the outer aspect of the femur and tibia.
Patients often report a fall with knee pain that prevents them from continuing the exercise they were doing. Many times, they describe hearing a pop, indicating a structural tear. In acute episodes, which are often initially classified as a knee sprain in emergency care, there is inflammation and joint effusion. Therefore, the doctor may decide to aspirate the knee (arthrocentesis) to remove the accumulated fluid, which in this case is mostly blood (hemarthrosis). Initially, partial immobilization of the knee, application of cold, some analgesic or anti-inflammatory medication, and rest are recommended.
When the patient consults a specialist, the most crucial aspect is the knee examination, as it plays a vital role in deciding the treatment. Whether or not surgery is necessary depends on how unstable or stable the orthopedic surgeon finds the joint to be. These maneuvers, called Lachman, Pivot-shift, and Anterior Drawer, provide information about the proper or improper functioning of the ligament, regardless of complementary imaging findings on Magnetic Resonance Imaging (MRI). In any case, an MRI is performed to confirm the appearance of the ligament and thoroughly assess other injuries to the meniscus or articular cartilage, which may themselves require surgical intervention.
If there are no other injuries, and the patient is not a regular athlete, conservative treatment can be considered since an isolated ACL tear does not cause pain and allows for a return to daily life in a few weeks. However, the leg must be strengthened significantly, and sports with a risk of injury, especially those involving rotational movements or sudden stops, must be avoided. In other words, a normal life can be resumed, including activities like cycling, swimming, and going to the gym without undergoing ACL surgery. However, this option is only suitable for middle-aged patients, as a knee without an ACL easily progresses to early osteoarthritis due to the distortion of normal knee kinematics.
For young and active patients, surgical treatment is the preferred option, involving ACL reconstruction since the ACL cannot be repaired. The various techniques used today are all arthroscopically assisted. The new ligament is created using either the patient’s own tendons (autograft) or a donor’s tendon (allograft). Tendons from the gracilis and semitendinosus (commonly called hamstring tendons) or the central third of the patellar tendon are often used. In the case of using a graft from a bone bank, the patellar tendon (BTB) or Achilles tendon is also commonly used. However, graft availability from bone banks is limited, and the risk of graft failure is higher. There is also the potential risk of transmitting viral diseases, but it is extremely rare given the stringent controls on tissues. When using an autologous graft, hamstring tendons are currently the most commonly used option because the morbidity in this area is minimal, and thigh and knee function does not seem to be affected.
The most important aspect of the surgery is the proper and as anatomical as possible placement of the new ligament. This is much more crucial than the choice of graft. Various grafts can be fixed in many ways, both in the femur and tibia, using interference screws, staples, cross-pins, or suspension systems. The surgeon will decide which ones to use based on the case and their experience. The surgery is not very long, approximately one hour, and can be performed under spinal or general anesthesia.
Patients we operate on usually spend one night in the hospital for pain control. If there are no concomitant cartilage lesions, we allow weight-bearing from the first moment. Quadriceps strengthening exercises and knee mobilization begin immediately. Once the sutures are removed in about 10-15 days, we start progressive rehabilitation of knee movement and strength.
One of the most feared complications is joint stiffness, which is mainly addressed with early mobilization. Infection or septic arthritis occurs in less than 1% of cases but can be a serious complication. To prevent thrombus formation in the venous system and fatal pulmonary embolism, the use of low molecular weight heparin is recommended.
Static cycling can be initiated in 2-3 weeks, a return to running is not advised before 2-3 months, and sports involving a risk of injury are typically not allowed before 4-6 months.
Currently, excellent functional and reproducible results are being achieved. There is a small percentage of cases in which knee revision surgery is required due to various reasons or graft failure in the future. In summary, approximately 85% of patients regain their pre-injury athletic level after this type of injury.
Rupture of the Posterior Cruciate Ligament of the Knee
Posterior Cruciate Ligament (PCL) and Knee Injuries
The posterior cruciate ligament (PCL) runs behind the anterior cruciate ligament (ACL) from the anterior and medial part of the femoral notch to the posterior region of the tibia.
Cruciate ligaments are crucial for the proper kinematics of the knee. PCL injuries occur due to falls directly onto the anterior part of the knee or in traffic accidents where the knee hits the dashboard. Whenever there is a knee dislocation, both cruciate ligaments are often seriously damaged.
In acute episodes, it is advisable to partially immobilize the knee, preferably with straight braces, apply cold, take some analgesic or anti-inflammatory medication, and, of course, rest.
When visiting a specialist, knee examination is the most critical aspect in deciding treatment. With maneuvers like the Posterior Drawer Test, Godfrey’s Relaxation Test, Quadriceps Test, Inverted Pivot Test, and External Tibial Rotation Test, the doctor obtains information about the proper or improper functioning of the ligament, regardless of complementary imaging findings on Magnetic Resonance Imaging (MRI). In any case, an MRI is performed to confirm the appearance of the ligament and thoroughly assess other injuries to the meniscus or articular cartilage, which may also require surgical intervention.
Isolated PCL injuries are rare. Unlike ACL injuries, most patients, including athletes, typically undergo conservative rather than surgical treatment for isolated PCL injuries. A PCL injury within the substance of the ligament, unlike the ACL, can heal with rest, and with the help of rehabilitation, knee stability can be restored.
In cases where stability cannot be improved with conservative treatment, and PCL incompetence persists, surgery is indicated for reconstruction, usually with a tendon graft from a bone bank. Surgery is also performed in cases of multiple injuries, especially those affecting the posterior and external region of the knee in addition to the PCL (when there is external knee instability). The most crucial aspect of surgery is the proper and as anatomical as possible placement of the new ligament. Various grafts can be fixed in many ways, both in the femur and tibia, using interference screws, staples, cross-pins, or suspension systems. The surgeon will decide which ones to use based on the case and their experience.
Surgery is performed under spinal anesthesia and with a thigh tourniquet to prevent bleeding during the operation. Patients we operate on usually spend one night in the hospital for pain control and go home with crutches and an articulated knee brace that must be worn for 4-6 weeks. If there are no concomitant cartilage lesions, we allow weight-bearing from the first moment. Once the sutures are removed in about 10-15 days, we start progressive rehabilitation of knee movement and strength. This process should be as long as necessary to achieve the desired activity level.
One of the most feared complications is joint stiffness, which is mainly addressed with early mobilization. Residual instability (especially external) is not uncommon. Infection or septic arthritis occurs in less than 1% of cases but can be a serious complication. To prevent thrombus formation in the venous system and fatal pulmonary embolism, the use of low molecular weight heparin is recommended.
These are severe knee injuries, and the results do not always allow a return to all types of sports.
Ankle Sprain and Instability
Ankle Anatomy and Sprains
The ankle joint is located between the distal ends of the tibia and fibula and the astragalus bone, hence its anatomical name, the tibioperoneoastragalar joint.
The ankle is the joint most commonly affected by twists or sprains and is one of the most frequent reasons for emergency trauma consultations.
It is a hinge-type joint with a wide range of flexion-extension motion (dorsiflexion and plantarflexion). Normally, dorsiflexion is about 15 degrees, and plantarflexion is about 30-40 degrees. Stability primarily depends on the position of the astragalus. When it is in extension (dorsiflexion), stability is greater due to the strong congruence of the articular surfaces. In plantarflexion, the collateral ligaments become more important as the astragalus is not as securely seated.
The medial ligament is called the deltoid ligament and is composed of several fan-shaped fascicles connecting the tibial malleolus to the medial region of the astragalus, the navicular, and the calcaneus. Injuries to this ligament are much less common.
The lateral ligament complex of the ankle is divided into three fascicles: the anterior talofibular ligament (ATFL), the calcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL).
The third stabilizing element besides bone shape and ligaments is the tendons that cross the ankle, acting as dynamic stabilizers and playing a vital role. The peroneal tendons are located on the lateral or external side, while the tibialis posterior tendon and the flexor tendons are in the medial or internal region.
In typical ankle sprains, the ankle is twisted inward in an inversion and plantarflexion motion, resulting in damage to the lateral ligaments. Typically, the ATFL is injured first, and if the motion continues, leading to forced varus of the ankle, the CFL may also be injured. PTFL injuries are less common and usually occur with direct or high-energy trauma.
Ankle sprains are clinically categorized into three grades:
- Grade I sprain: There is mild stretching or partial tearing of the ligament fibers.
- Grade II sprain: There is significant partial tearing of the ligament, but continuity is maintained. Most cases fall into this category.
- Grade III sprain: There is a complete ligament tear with anterior and varus instability.
The treatment of ankle sprains is typically conservative, but improper management can lead to prolonged pain or recurrent sprains.
In Grade I sprains, relative rest and classic measures such as elevation, compression, and local cold application are usually sufficient.
Grade II sprains are a diverse group with varying outcomes, often complicated by associated injuries. Currently, it is recommended to immobilize the ankle briefly until pain subsides. Weight-bearing with crutches is allowed early. Traditionally, these injuries were immobilized for 3-4 weeks in a cast, unnecessarily prolonging recovery.
Physical therapy initially aims to control inflammation and later promote ligament healing and proper function, with a focus on strengthening dynamic stabilizers and proprioception.
In Grade III sprains, initial treatment can be similar to Grade II, with slightly longer immobilization. However, if the ankle is unstable on examination, ligament repair surgery may be necessary. Associated injuries (fractures, osteochondral lesions, etc.) can also occur in these cases. An MRI evaluation is recommended, and surgery may be necessary. In high-level athletes, where the risk of persistent instability is high (especially in sports like basketball, handball, and soccer), direct surgical treatment may be beneficial, allowing for a faster return to competition.
In the initial assessment of an injured ankle, simple X-rays should be taken to rule out ankle fractures, which often require intervention. Another common injury in foot twists is the fracture of the base of the fifth metatarsal, which will be discussed separately. Some patients may have suffered dislocation of the peroneal tendons, but this is not easy to detect in the emergency department.
To rule out other injuries that may have occurred during the twist, an MRI can be ordered in cases where recovery is not satisfactory within the first few weeks. These images often show bone edema in the astragalus and malleoli, resulting from bone contusion. While these injuries have a good prognosis, recovery is typically slow and often causes persistent pain in the early weeks. Cartilage injuries and osteochondritis of the astragalus may require surgical treatment if they are unstable. Occasionally, non-displaced fractures of the astragalus, calcaneus, or cuboid may be discovered.
A rare but highly challenging complication is the development of Complex Regional Pain Syndrome (formerly called Reflex Sympathetic Dystrophy or Südeck’s syndrome). It involves permanent pain and functional impairment over several months, necessitating extensive rehabilitation and having a significant psychological impact on those affected.
Sometimes, after an initial sprain, the patient starts experiencing recurrent twists. If we detect anterior and external ankle instability during the examination, we are dealing with a condition known as ankle instability.
The lack of function in the lateral ligaments of the ankle, typically the ATFL and CFL, is often the cause of instability. A severe initial trauma and poor recovery after the initial episodes, without adequate focus on dynamic stabilizer exercises, usually worsen the problem. Stability can be objectively assessed by an experienced physician during physical examination. Imaging tests such as X-rays, bone scans, or MRI can help evaluate the ankle comprehensively but do not directly identify instability. The ligaments may be visible on MRI or ultrasound images, but the patient’s history and instability detected during examination lead to the diagnosis.
If the patient wishes to continue participating in high-risk ankle injury sports, the best treatment is surgical. In patients who simply want to lead a normal life with some exercise, such as cycling, swimming, elliptical training, or other controlled exercises, the need for surgery will depend on whether they experience frequent ankle sprains, even in everyday life.
In cases of doubt and in cases of inadequate initial rehabilitation, we recommend rehabilitation as the first option. This rehabilitation should focus on ankle strength, balance, and proprioception. Working on the peroneal tendons is crucial because their contraction opposes the movement that typically causes injury. If the patient continues to experience twists and discomfort after completing rehabilitation, surgical intervention may be considered, but it is usually postponed for up to 6 months before making that decision.
Regarding surgical technique, whenever possible, an anatomical repair with tensioning of the ATFL and CFL is performed, using suture anchors (Bröstom-Gould technique).
After this surgery, performed under spinal or general anesthesia, the ankle is kept in a splint for 2-3 weeks, followed by immobilization in a cast or brace for an additional 2-3 weeks.
Rehabilitation for flexion and extension usually begins between one and six weeks. Normal activity should not resume before 2-3 months, and high-risk sports should be avoided for up to 6 months.
In cases of severe ligament damage or when there is a failure of previous intervention, reconstruction of the ligaments with the lateral short peroneal tendon or autograft of the semitendinosus tendon (obtained from the patient’s knee during the same surgical procedure) may be an option. The postoperative process is similar in both cases.
The results are satisfactory in the vast majority of patients, and ankle stability is restored. In some patients with other associated joint injuries, an ankle arthroscopy is performed in the same procedure to address them.
Bone Injuries
Clavicle fracture
Clavicle fractures are some of the most common injuries in the world of sports. Falls onto the shoulder are the main cause, especially in cycling, motorcycling, skiing, and contact sports. The clavicle bone follows a smooth double-curved path, and at its lateral end, it articulates with the acromion of the scapula. This joint, the acromioclavicular joint, is also frequently injured in falls or similar impacts, but in this case, it’s the acromioclavicular and coracoacromial ligaments that are affected. These injuries deserve a separate discussion.
The area where the clavicle is most frequently fractured is its middle part. Typically, the medial or inner fragment ascends and becomes prominent under the skin, while the lateral fragment tends to descend, causing shortening of the clavicle. Occasionally, there are three or more fragments, especially in fractures resulting from high-energy mechanisms.
Diagnosis is straightforward through physical examination of the patient. Plain X-rays are essential to precisely determine the type of fracture and plan the definitive treatment. Other complementary tests are usually unnecessary.
Conservative treatment involving immobilization with a figure-of-eight bandage or sling yields good results in most cases. However, it has the drawback of not achieving anatomical reduction of the fracture and can be uncomfortable to wear. If the patient needs to return to physical activity quickly, surgical intervention may be necessary. For patients with no urgent need to return to exercise, orthopedic treatment is still recommended, unless there is skin compromise due to significant displacement.
The most commonly used surgical technique today is open reduction of the fracture and internal fixation with a plate and screws. Specifically designed plates for this location are now available. Complications of this procedure, typically performed under general anesthesia, include infection or wound dehiscence (rare) and loss of sensation in the upper torso territory due to damage to cutaneous branches in the incision area (common).
Following surgery, a sling is used for two weeks, and immediate movements of the elbow and wrist are allowed, while shoulder movement is restricted to 90º of abduction. Rehabilitation begins after suture removal at 10-15 days.
Both operated and non-operated clavicle fractures carry the risk of non-union, leading to clavicular pseudoarthrosis. Non-union is more common in non-operated patients. In cases where non-union is painful, surgical intervention is necessary. Apart from appropriate plate and screw osteosynthesis, bone grafting or other aids to promote healing in the area may be required.
Traditionally, clavicle fractures have predominantly been treated without surgery. In recent years, there has been a growing trend towards surgical intervention because patients demand faster recovery and greater reliability in fracture union. Additionally, it has been observed that in highly displaced fractures with shortening, the mechanics of the shoulder girdle are altered, and only surgery can restore clavicle length.
Tarsal Scaphoid Stress Fracture
The scaphoid bone, also known as the navicular bone, is located in the midfoot, between the head of the talus and the three cuneiform bones. It has a prominent medial tuberosity where the tibialis posterior tendon inserts. It is a bone that occupies the center of the longitudinal arch of the foot.
Load forces are transmitted from the toes and metatarsals to the cuneiforms and from there to the scaphoid and talus. The talonavicular joint has mobility in all planes of space, and its movement, combined with the subtalar joint, is essential for foot inversion and eversion.
Fractures of the scaphoid bone typically occur slowly, causing mild symptoms that do not necessarily prevent the individual from continuing their activity. Patients may experience ankle and foot pain, often without any recognized trauma, and may even develop a limp. It is common for people not to initially suspect a bone injury and instead think it’s a tendon issue. Athletes are often treated by physiotherapists before a diagnosis is made.
Cases of scaphoid fractures have been observed in various sports, including tennis, soccer, and basketball. It is a common injury among middle-distance runners who combine speed training with high mileage.
If the injury is not detected early, the bone overload can progress to a fracture line, typically located at the junction between the two-thirds medial and one-third lateral of the bone, right in the center of the instep. The direction of this fracture is longitudinal and extends plantarly, sometimes resulting in a complete and displaced fracture.
Diagnosis using plain X-rays is difficult unless there is a complete fracture. When the initial symptoms arise and there is suspicion of a scaphoid fracture, an MRI should be requested, which will reveal osteoblastic reaction secondary to the injury and bone edema.
A CT scan can also help define the severity of the injury once it has been diagnosed, and treatment options may depend on the timing of diagnosis.
In the early stages with a normal X-ray but a diagnosis confirmed by bone scan or MRI, and in the absence of a clear fracture line, discontinuing sports activity might be sufficient, although in some cases, immobilization with a cast or walker for six weeks may be preferable.
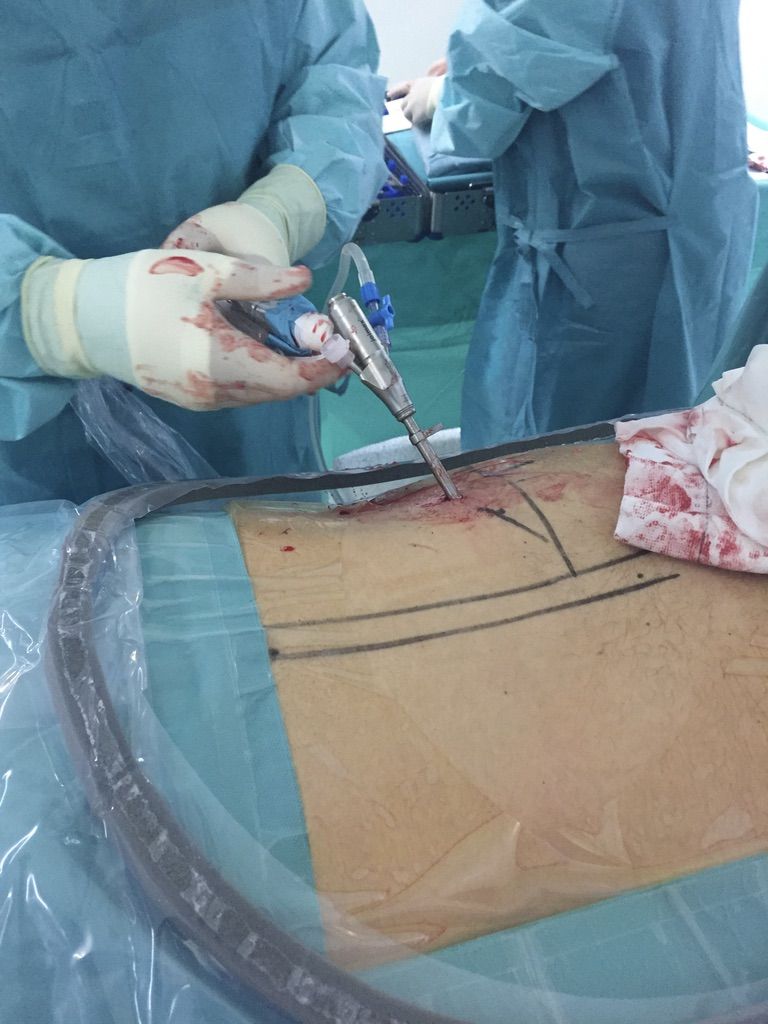
In our opinion, complete fractures should undergo surgical treatment because it allows for the reduction of any displacement, no matter how small, increasing the chances of consolidation and enabling earlier mobility, which is crucial for an athlete. Surgery can be performed percutaneously, with the placement of a compression screw in the scaphoid bone under radiological guidance.
In cases of long-standing injuries, the likelihood of pseudoarthrosis or non-union of the bone is high. To address this complication, surgery is required, including the opening and cleaning of the focus, along with fixation using a screw.
Most affected athletes can recover their sports performance level after a few months of progressive rehabilitation following the immobilization and off-loading phase.
Clinic
Medical Centre
MedHelp Marbella
medhelpmarbella@gmail.com
Appointment Times
Mon-Fri: 9:30-3:00pm
Mon & Thur: 4:00-8:00pm